
Dr Kieron Lim
Consultant Gastroenterologist & Hepatologist
MBBS, University of London, Member, Royal College of Physicians (UK), Fellow, Academy of Medicine (Gastroenterology) Singapore, Fellow, Royal College of Physicians (Edinburgh)
What Is Liver Cirrhosis?
Liver cirrhosis is a late stage of liver disease where healthy liver tissues are replaced with scar tissues. Each time your liver is injured, it tries to repair itself. In the process of doing so, scar tissue forms. As more and more scar tissue forms, it makes it harder for the liver to function properly.
As this scar tissue builds up, it begins to disrupt blood flow and impair the liver’s ability to process nutrients, hormones and toxins. Cirrhosis is a progressive condition and, in later stages, may lead to liver failure and serious health complications.
What Causes Liver Cirrhosis?
Cirrhosis of the liver can be attributed to various factors, such as:
Viral Hepatitis B and C
Chronic infection with hepatitis B or C viruses can lead to liver inflammation and, over time, the development of liver cirrhosis.
NAFLD and NASH
Accumulation of fat in the liver can progress to non-alcoholic fatty liver disease (NAFLD) or non-alcoholic steatohepatitis (NASH) and eventually to liver cirrhosis.
Chronic Alcoholism
Prolonged and excessive alcohol consumption can cause liver inflammation, fibrosis, and ultimately alcoholic liver cirrhosis, posing a substantial risk to liver health.
Genetic Disorders
Certain genetic conditions, such as hemochromatosis and Wilson's disease, can predispose one to liver cirrhosis due to impaired liver function.
Autoimmune Liver Diseases
Conditions such as autoimmune hepatitis and primary biliary cholangitis, cause the immune system to attack the liver, resulting in inflammation and scarring.
Chronic Bile Duct Disorders
Diseases affecting the bile ducts, such as biliary atresia or chronic bile duct obstruction, can lead to liver cirrhosis over time.
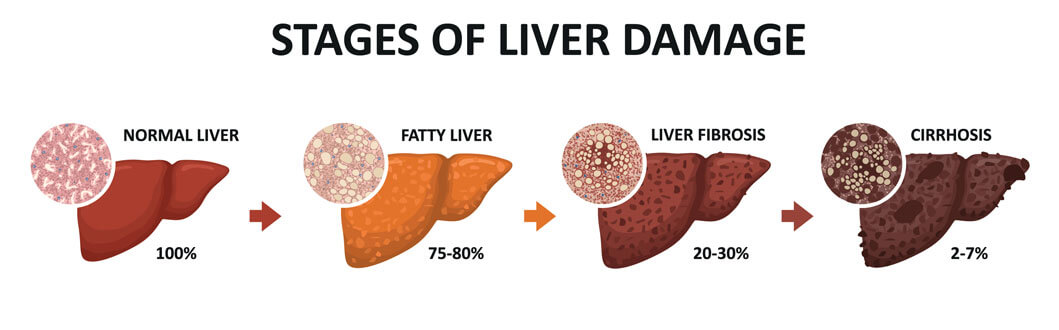
What are the Stages of Liver Disease?
Liver disease progresses through several stages, each marked by specific changes in liver health and function.
Stage 1: Steatosis
The initial stage is characterised by the inflammation of the bile duct or liver. Symptoms typically include abdominal discomfort. Symptoms and inflammation are generally treatable at this stage. However, if left untreated, this inflammation can lead to liver damage.
Stage 2: Fibrosis
Liver disease is frequently identified during the second or third stage when symptoms become more apparent. At this point, scarring or inflammation begins to impede blood flow in the liver, affecting its function. However, with appropriate treatment, the liver retains the potential to recover.
Stage 3: Cirrhosis
The third stage, known as cirrhosis, represents the advanced stage of liver disease, primarily resulting from untreated inflammation and scarring. Over time, healthy liver cells are replaced by scar tissue, leading to permanent scarring and hardening of the liver. As scar tissue accumulates, liver function diminishes, making blood flow through the liver difficult.
Stage 4: Liver Failure or Advanced Liver Disease
The final stage signifies the end stage of the disease, where the liver loses its ability to function effectively. Prompt medical intervention is necessary at this stage to prevent fatalities and manage complications associated with liver failure.
What Are the Symptoms of Early-Stage Liver Cirrhosis?
- Persistent tiredness and weakness (fatigue)
- Nausea and vomiting
- Loss of appetite and weight loss
- A general feeling of discomfort or illness (malaise)
- Upper abdominal pain
- Swelling in the abdomen, ankles, or legs
- Red patches on the palms
- Small, spider-like blood vessels on the skin (spider angiomas)
What Are the Symptoms of Advanced Liver Cirrhosis?
- Yellowing of the skin and whites of the eyes (jaundice)
- Swelling in the abdomen (ascites)
- Swollen legs (oedema)
- Dark-coloured urine and light-coloured or bloody stool
- Vomiting blood
- Motor dysfunction
- Itchy skin without visible rash (pruritus)
- Confusion, disorientation, or mood changes (encephalopathy)
What Are Possible Complications of Liver Cirrhosis?
If left untreated, complications may include:
- High blood pressure in the liver (portal hypertension)
- Increased risk of liver cancer (hepatocellular carcinoma)
- Mental confusion caused by toxin buildup in the blood and brain (hepatic encephalopathy)
How Is Liver Cirrhosis Diagnosed?
A liver specialist typically diagnoses cirrhosis using the following tests:
Blood Tests
Blood tests play a crucial role in assessing liver function and identifying markers of liver injury, such as elevated liver enzymes, bilirubin levels, and abnormal clotting factors.
Imaging Tests
Imaging modalities like ultrasound, CT scan, or MRI can help visualise changes in liver structure, detect the presence of nodules or masses, and assess the extent of liver fibrosis.
Liver Biopsy
A liver biopsy may be performed to obtain a tissue sample for microscopic examination, providing detailed information about the degree of fibrosis, inflammation, and any underlying liver disease.
Liver Stiffness Measurement (Transient Elastography)
This non-invasive technique measures liver stiffness, serving as an indirect marker of liver fibrosis and cirrhosis, aiding in disease staging and treatment planning.
What Are the Types of Liver Cirrhosis Treatments?
Liver cirrhosis treatment involves a multifaceted approach aimed at addressing the underlying causes, managing complications, and preserving liver function. Treatment options include:
Lifestyle Modification
Adopting a healthy lifestyle, including a balanced diet, regular exercise, and avoiding harmful substances.
Alcohol Abuse Treatment
For individuals with alcohol-related liver cirrhosis, abstaining from alcohol is essential.
Non-Alcoholic Fatty Liver Disease Treatment
Managing conditions such as non-alcoholic fatty liver disease involves lifestyle modifications, weight management, and controlling associated risk factors like diabetes and high cholesterol.
Hepatitis Treatment
Treating viral hepatitis (such as hepatitis B and C) with antiviral medications can help prevent liver damage.
Liver Transplantation
In advanced cases of cirrhosis where liver function is severely compromised, liver transplantation may be considered to replace the diseased liver with a healthy donor organ.
Can Liver Cirrhosis Be Prevented?
While some causes of liver cirrhosis are not entirely preventable, adopting a healthy lifestyle can help. These include:
Limit Alcohol Consumption
Excessive alcohol consumption is a leading cause of alcoholic liver cirrhosis. Limiting alcohol intake or abstaining entirely can prevent liver damage and cirrhosis.
Maintain a Healthy Diet
Eating a balanced diet rich in fruits, vegetables, lean proteins, and whole grains can help maintain liver health and prevent conditions like non-alcoholic fatty liver disease (NAFLD), which can progress to cirrhosis.
Manage Chronic Conditions
Conditions such as obesity, diabetes, and hepatitis B and C can increase the risk of liver cirrhosis. Proper management of these conditions through medication, lifestyle changes, and regular medical care can reduce the risk of cirrhosis.
Protect Yourself From Hepatitis
Practising safe sex by using condoms and avoiding sharing needles can reduce the risk of contracting certain types of hepatitis.
Get Vaccinated
Vaccination against hepatitis B can prevent infection and the resulting liver damage.
Regular Medical Check-ups
Regular monitoring of your liver health can help detect any early signs of liver damage or disease for prompt intervention before it progresses into cirrhosis.
Frequently Asked Questions (FAQs) About Liver Cirrhosis
Can liver cirrhosis be reversed?
What happens if liver cirrhosis is left untreated?
What is the difference between liver fibrosis and liver cirrhosis?
How often should I see a specialist if I have liver cirrhosis?

Meet Our Liver Cirrhosis Specialist
Dr Kieron Lim
MBBS, University of LondonMember, Royal College of Physicians (UK)Fellow, Academy of Medicine (Gastroenterology) SingaporeFellow, Royal College of Physicians (Edinburgh)
Dr Kieron Lim is a senior consultant specialising in Gastroenterology and Hepatology, and the Medical Director of the Liver Transplant Programme at Mount Elizabeth Hospital. With in- depth experience in the field, Dr Lim is known for his excellent patient care for individuals with liver fibrosis, liver cirrhosis, viral hepatitis B and C, fatty liver disease, and liver cancer. His expertise also extends to conducting endoscopic procedures such as diagnostic oesophago-gastro- duodenoscopy (OGD), colonoscopy, and liver transient elastography (FibroScan).


